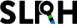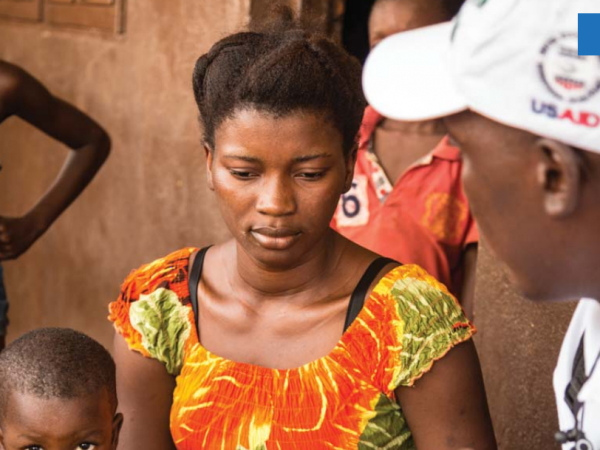
Sierra Leone Malaria Control Strategic Plan (2016- 2020)
The Government of Sierra Leone recognises malaria as a health and socioeconomic burden as articulated in the National Health Sector Strategic Plan (NHSSP 2010-2015), Sierra Leone Health Recovery Plan 2015–2020, National Ebola Strategy for Sierra Leone 2015-2017 and the Basic Package of Essential Health Services 2010 (revised 2015). Malaria is endemic in Sierra Leone with stable and perennial transmission in all parts of the country. Malaria is presently the leading cause of morbidity and mortality amongst children under five years of age. Although pregnant women and children under 5 are mostly affected, the entire population is risk of malaria. Malaria accounts for 40.3% of outpatient morbidity for all ages. Accounts for 47% of outpatient morbidity for under five children and accounting for 37.6% for hospilisation with a case fatality of 17.6% (sources). Malaria and poverty are closely linked. Malaria is concentrated in low income and lower income countries. Within these countries, the mostly severely affected communities are those that are the poorest and most marginalised. Such communities have the highest risks associated with malaria, and the list access to effective services for prevention, diagnostics and treatment. Malaria is a major threat to socio-economic development of the country with an estimated 7-12 days lost on the average per episode of malaria. It imposes substantial costs to individuals, households and governments. The cost to individuals and their family includes purchase of drugs for treating malaria at home; expenses to travel to and seek treatment at dispensaries and clinics; lost days of work; absence from school; expenses for preventive measures; expenses for burials in case of deaths. Households in Africa spend between $2 and $25 (USD) on malaria treatment and between $15 and $20 on prevention each month with consequent loss of resources or 3% of annual income. The amount spent on malaria in terms of prevention, treatment and loss of productivity can compromise significant portion of annual income of poor households. Furthermore, severe malaria impairs children’s learning and cognitive abilities by as much as 60%, consequently affecting the performance of Sierra Leone’s universal primary and secondary education programmes. This Sierra Leone Malaria Strategic Plan covers the 2016-2020 period. The plan stipulates priority interventions, outlines the strategic direction and the investments required for achieving the 2020 national goals. The strategic plan also outlines how the stakeholders in malaria control 1.1. Introduction Sierra Leone Malaria Control Strategic Plan 2016-2020 pg. 22 will organize themselves in achieving the objectives and goals set herein as informed by the midterm review and the other related strategic documents. In addition this plan will be a resource mobilization tool and will provide a common framework for the accelerated nationwide scale up of evidenced‐led malaria reduction interventions by the government, its development partners, the private sector and all stakeholders.
The health sector has to be viewed within the broad historical context of poverty and a high illiteracy rates in Sierra Leone (43%). Sierra Leone is recovering from multiple disasters: the civil war (1990–2002); the cholera epidemic (2012); and the EVD outbreak (2014-2015). The country was deemed to have “not attained the minimum International Health Regulations core capacities by 2012”. Nevertheless, prior to the EVD outbreak in mid-2014, Sierra Leone had made substantial progress towards a number of the Millennium Development Goal targets in the health and nutrition sectors, including a reduction in child and maternal mortality and improving coverage with a range of critical interventions such as malaria control, antenatal care, skilled birth attendance and immunization. The recent national Malaria Indicator Survey (2013) and the Demographic Health Survey (2013) also demonstrated major improvements in malaria control. Framed alongside commitments articulated in the national development plans, the National Health Strategic Plan 2010–2015, the Health Sector Strategic Plan 2015-2020, Free Health Care 2010, the Basic Package of Essential Health Services 2010 (Revised 2015), the National Health Compact 2011 and the Service Level Agreement (2015) provide the overall guidance for health system strengthening and for improving the health status of the population. Health policies, programmes and coordinating structures, such as the Health Sector Coordinating Committee chaired by the Minister of Health and Sanitation, do exist, galvanizing cooperation among health, environment and development partners in the country. The Sierra Leone Malaria Strategic Plan (SLMSP) shall follow the principles of the Paris Declaration and the Accra Agenda for action for Aid effectiveness through the International Health Partnership (IHP+) in the interaction and collaboration with national and international development partners as embedded in the health sector strategic plan. Malaria control has remained a priority action within the national health agenda in Sierra Leone. The country has favourable policies to ensure that malaria is controlled in the country. User fees were abolished in all public and few private health facilities making treatment free for malaria cases and government taxes on Long Lasting Insecticides Treated Nets (LLINs), medicines and laboratory supplies were also waived in 2005. Furthermore, the government is committed to the 2006 World Health Assembly (WHA) resolution to withdraw Artemisinin monotherapy. At the highest level, His Excellency the President is an active member of the African Leaders Malaria 1.2. National and international context and commitments Sierra Leone Malaria Control Strategic Plan 2016-2020 pg. 23 Alliance (ALMA). In order to ensure that malaria control is on the national agenda, a Parliamentary Health Committee was formed. The country has embraced global and regional commitments in malaria prevention and control. The African Union Heads of State jointly stated their commitment in 2000 during the Abuja Declaration, calling for “Universal Access” to HIV/AIDS, Tuberculosis and Malaria services by 2010. All policies and strategic plans have always been aligned to the World Health Organisation (WHO) guidelines, Roll Back Malaria (RBM) and Millennium Development Goal (MDG) targets. Following the United Nations Secretary General’s call for 100% coverage of malaria control interventions and the elimination of malaria as a threat to public health, the government of Sierra Leone has moved from targeting of malaria control interventions to universal coverage.
National Community Health Worker Policy (2016 -2020)
Sierra Leone’s National CHW Programme has been in formal existence since 2012, when the MOHS, supported by partners, developed the fi rst national CHW policy focused on providing a basic package of services at the community level. This national programme was built on decades of eff orts to bring essential services to communities across the country through a variety of vertical community-based programmes, such as Traditional Birth Attendants (TBAs), Community Drug Distributors through the Neglected Tropical Diseases Programme, Community-Based Providers through the National Malaria Control Programme (NMCP), and Blue Flag Volunteers diagnosing and treating diarrhoea. Additionally, many NGOs promoted community-based care through Community-Based Workers and volunteers. These programmes demonstrated the importance of providing care at the community level.

Until the Ebola outbreak, the implementation of the 2012 National CHW Policy was on track to achieve results for mothers and children in Sierra Leone. However, the support to CHWs during the Ebola outbreak was signifi cantly aff ected by less supportive supervision and decreased stock of supplies. In addition, the CHWs were called to perform additional tasks during the outbreak, including contact tracing, Community Event-Based Surveillance, and social mobilization on Ebola related messages. In some instances, CHWs even served as burial team members. In order to take into account the lessons learned from the 2012 Programme and from CHWs work during the Ebola outbreak, the MOHS and partners embarked on revising the 2012 policy. The 2016 CHW Policy builds on the historic eff orts to strengthen and harmonize diff erent community-based programmes to provide comprehensive primary health care at the community level. This revised and updated policy provides further guidance on coordination, implementation, and monitoring and evaluation of the National CHW Programme; CHWs’ revised Scope of Work (SOW); geographical coverage; selection criteria and processes; supervision; incentives and remuneration; expanded standardized training curriculum; supplies; and reporting. The National CHW Programme aims for national scale so that all hard-to-reach communities receive a basic but comprehensive package of services. The 2016 National CHW Policy provides guidance on the minimum package of services to be provided by CHWs and the minimum package of inputs required to support those CHWs. All Ministry programmes and directorates, partners, and donors working to implement and support the National CHW Programme must meet the minimum standards outlined in this policy. The National CHW Programme looks forward to working with other MOHS programmes, Implementing and Technical Partners, and communities over the coming years to build a strong National CHW Programme that serves the needs of communities, is accountable to those it serves, and improves the health of all Sierra Leoneans. Policy revision process The MOHS, led by the Directorate of Primary Health Care (DPHC), with support from the Health Systems Strengthening Hub and UNICEF, began revising the National CHW Programme in March 2015. This included a series of consultations with the MOHS, other line ministries, Technical Partners and Implementing Partners (IPs), as well as a workshop with key stakeholders such as Local Councils, partners, and civil society and international representatives to consider evidence and best practices. A series of small working groups were later created to discuss key areas, and consisted of partners and MOHS staff . The National CHW Technical Working Group (TWG) contributed to these discussions throughout the policy revision process. Based on evidence gathering and discussions, draft recommendations were written in November 2015 and presented to the TWG and MOHS directorates, programmes, and leadership. A fi nal policy was drafted in February 2016 by the National CHW Hub and Technical Advisors. The policy was reviewed by the Steering Committee and validated by all key stakeholders before being fi nalized in August 2016. Vision, mission, guiding principles, and Programme objectives Vision The National CHW Programme aims to support a functional CHW programme that is part of a resilient national health system. The Programme aims to provide effi cient, basic, and high-quality services that are accessible to everybody, especially people living in hard-to-reach areas. Mission CHWs contribute to the Agenda for Prosperity: Road to Middle-Income Status (2013–2018) and socio-economic development by promoting access to high-quality health care, including reproductive health care and nutrition services, for the population of Sierra Leone. Guiding principles The National CHW Programme, which is led by the Government of Sierra Leone through the MOHS, is guided by the following key principles: 1. Save lives, particularly those of pregnant and post-natal women, newborns, and children under fi ve. This will be achieved by ensuring that the National CHW Programme provides complimentary services as part of an overall health system strengthening approach that seeks to deliver high-quality preventive and curative services at the community level while making referrals as needed. 2. Create an ongoing, evidence-based learning and policy environment that can infl uence programmatic changes that refl ect the national and international health landscape while responding to potentially changing local situations. 3. Encourage community engagement and ownership to ensure that the National CHW Programme meets the needs of and is accountable to the communities it serves. Foster individual and community health care service utilization and ownership of health outcomes. 4. Foster partnership, coordination, and mutual respect among all stakeholders from Community Members and CHWs to Donors and Development Partners. Commit to strong communication, transparency, accountability, and iterative learning throughout the Programme. 5. Ensure complementarity—not duplication—of services and eff orts at community, district, and national levels. Ensure joint and proper planning of the Programme with other MOHS structures and Health and Development Partners. 6. Ensure that community-based services are equitably off ered and accessed across Sierra Leone. Policy review and update The MOHS, with support from partners, commits to reviewing and updating this policy as needed. The National TWG and Steering Committee will review this policy and the associated strategy at least annually. Any changes will be formally adopted by the MOHS and included as an addendum.Key stakeholders Ministry of Health and Sanitation Directorate of Primary Health Care The National CHW Programme is part of the MOHS. Within the MOHS, the DPHC, through the National CHW Hub, oversees and is responsible for ensuring that the policy and strategy are implemented and in place. The DPHC must also ensure coherence and complementarity between the National CHW Programme and other programmes within the MOHS. Within the DPHC, the National CHW Hub is the coordinating body for CHW activities nationwide and is responsible for: • Overseeing implementation and monitoring of the CHW Programme • Overseeing Programme quality • Overseeing coordination between key stakeholders, including other MOHS programmes and non-MOHS partners • Fundraising and allocation of resources • Supporting an enabling environment for CHWs and the Programme • Ensuring alignment of the CHW Programme with health and development goals, strategies, and policies • Identify research needs and oversee operational studies and evaluations\ CHW Steering Committee The CHW Steering Committee is chaired by the Director of Primary Health Care, with the National CHW Hub serving as the Secretariat. Members include all MOHS Directors and Programme Managers whose programmes are implicated in the National CHW Programme, including but not limited to the National Malaria Control Programme (NMCP), Disease Surveillance Control Programme, Food and Nutrition Directorate, Reproductive and Child Health Directorate, National TB/ Leprosy Control Programme and National AIDS Control Programme, and the Directorate of Human Resources for Health. The Steering Committee is responsible for overseeing implementation of the National CHW Programme, ensuring that goals and timelines are met, as well as fi nding solutions to implementation, funding, and governance diffi culties. The Steering Committee is also responsible for developing and ensuring implementation of an integration strategy, and supports coherence and complementarity between the CHW and other MOHS programmes. District Health Management Teams DHMTs are responsible for district-level planning, implementation and monitoring of the National CHW Programme in line with the National CHW Policy. This may be in the form of direct implementation through the DHMT staff and MOHS structures, and/or collaborating with IPs to do so. The DHMT maintains a database of all active CHWs in the districts, offi cially certifi es and registers them, and ensures that they have the support needed to fulfi l their roles. Other line ministries As the Government of Sierra Leone increases ownership of the National CHW Programme, the involvement of other line ministries, such as the Ministry of Finance; the Ministry of Local Government; the Ministry of Social Welfare, Gender and Children’s Aff airs; the Ministry of Trade and Industry; and the Ministry of Education, will be essential. Local governance Traditional leaders Chiefs and other traditional leaders help CHWs to promote healthy and health-seeking behaviours in their communities. They are responsible for ensuring community ownership and functionality of community level structures. They need to make sure that CHWs and/or their Peer Supervisors are represented in the community structures so that CHWs will report their challenges and successes to initiate appropriate actions. Local and District Councils Local and District Councils are responsible for supporting implementation of the National CHW Programme at the district level, including ensuring that the Programme interacts with other local structures, particularly local governance structures.